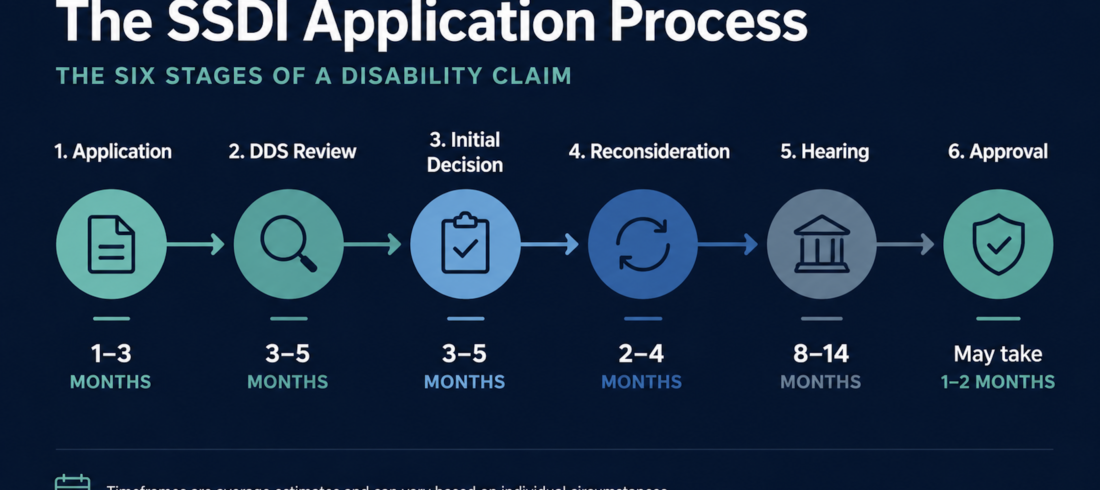
You got approved. After everything that went into getting here, the paperwork, the waiting, the uncertainty, that letter finally said yes. Take a moment with that. It’s a big deal and you earned it.
Now let’s talk about what comes next. Because the approval letter is the beginning of a new set of things to understand, not the end of the process entirely. The first 90 days after approval involve decisions, timelines, and information that most people have to figure out on their own. This guide covers all of it.
Your First Payment: When It Actually Arrives
This is the first thing everyone wants to know. And the honest answer is that it depends on a few things.
SSDI has a mandatory five-month waiting period built into the program. It applies to almost everyone. The SSA does not pay benefits for the first five months after your established onset date, which is the date they determined your disability began. If your claim took a long time to process, there’s a good chance those five months already passed during the application period. In that case your first payment may arrive relatively quickly after approval.
If your onset date was established recently, the five months may not have elapsed yet. Your payment start date gets pushed out accordingly.
The approval letter should spell out your payment start date and your monthly benefit amount. Read that section carefully. If the numbers don’t make sense or the timeline seems off, call the SSA to get clarification. The number is 1-800-772-1213.
SSDI pays one month behind. Benefits for January arrive in February, for example. The SSA processes payments on a schedule based on your birth date. If your birthday falls between the 1st and 10th of the month, payments come on the second Wednesday. Between the 11th and 20th, the third Wednesday. Between the 21st and 31st, the fourth Wednesday. Mark that on your calendar so you know when to expect deposits going forward.
Back Pay: The Lump Sum and What to Expect
If there was a significant gap between your filing date and your approval, you’re likely owed back pay. This arrives separately from your first regular monthly payment, typically as a lump sum direct deposit. It doesn’t always come at the same time as your first monthly check. Sometimes it arrives a few weeks before, sometimes after. The SSA processes them independently.
The amount is calculated from your established onset date, minus the five-month waiting period, up to a maximum of twelve months before your filing date. For someone who waited a year or more for approval, that back pay check can be substantial.
A few things worth knowing about back pay. If you had an attorney or advocate representing you, their fee comes out of the back pay before it reaches you. The SSA pays them directly. The fee is capped by federal law at 25 percent of back pay up to a set maximum, so there are no surprises there, but factor it in when you’re thinking about what to expect.
If you also receive SSI in addition to SSDI, back pay rules work differently for the SSI portion. SSI back pay above a certain threshold gets paid in installments rather than a lump sum. Your approval letter should address this if it applies to your situation.
Setting Up Direct Deposit
If you didn’t set up direct deposit during the application process, do it now. The SSA strongly prefers electronic payment and it’s faster and more reliable than a paper check. You can set it up through your my Social Security account at ssa.gov or by calling the SSA directly. You’ll need your bank’s routing number and your account number.
If you don’t have a bank account, a Direct Express prepaid debit card is an option the SSA offers specifically for benefit recipients. It functions like a debit card and gets loaded automatically on payment dates.
Medicare: The Part Nobody Warns You About
Here’s the thing that catches almost everyone off guard. Approval for SSDI does not mean you have Medicare right now.
There is a 24-month waiting period for Medicare coverage that begins from your first month of SSDI entitlement, meaning the month your benefits officially began, not the month you were approved. Two full years. During that window you are responsible for your own health coverage.
If you had employer coverage through a spouse or family member, staying on that plan during the waiting period is often the most straightforward option. COBRA continuation coverage from a former employer is another possibility, though it tends to be expensive. Marketplace coverage through healthcare.gov is worth looking into, particularly if your income is low enough to qualify for subsidies. Medicaid is also available in most states for people with limited income and assets, and unlike Medicare, it has no waiting period.
The 24 months goes faster than it sounds, especially once you’re settled into a routine. But plan for it. Don’t assume Medicare coverage starts immediately and then get caught without insurance when a medical bill arrives.
There is one exception worth knowing. If your disability is ALS, also called Lou Gehrig’s disease, the Medicare waiting period is waived entirely. Coverage begins the same month SSDI entitlement begins.
What to Do About Health Insurance Right Now
Given the Medicare gap, this deserves its own conversation. Your options depend on your specific situation but here’s a practical breakdown.
Check whether you qualify for Medicaid first. In states that expanded Medicaid under the Affordable Care Act, eligibility is based primarily on income. If your only income is SSDI and it falls below the threshold for your state, you may qualify immediately. Coverage through Medicaid can run concurrently with SSDI and then transition to Medicare coordination once your 24 months is up.
If you don’t qualify for Medicaid and need coverage, go to healthcare.gov and run the numbers on a marketplace plan. SSDI income counts as income for subsidy calculations, but at many benefit levels, subsidies bring premiums down to a manageable range. Open enrollment happens annually but a new SSDI approval qualifies as a special enrollment event, so you can enroll outside the standard window.
Reporting Requirements: What You Have to Tell the SSA
Being on SSDI comes with ongoing reporting obligations. Missing them has real consequences. Here’s what the SSA needs to hear from you.
Any return to work. This is the big one. If you start working at all, the SSA needs to know. Even if it’s part-time, even if it’s just a few hours a week. The rules around working while on SSDI are more nuanced than most people expect, but the SSA needs to be in the loop from the start.
Changes in your medical condition. If your condition improves significantly, you’re supposed to report that. If it worsens and you need different treatment or have a new diagnosis, that’s also worth documenting with the SSA.
Changes in living situation. Getting married or divorced, someone moving into or out of your household, a change of address. All reportable.
Changes in income from other sources. Workers’ compensation, certain pension payments, and other government benefits can affect your SSDI amount. The SSA needs to know if those circumstances change.
The safest approach is to err on the side of reporting more rather than less. Oversharing with the SSA costs you nothing. Failing to report something that should have been reported can result in an overpayment that you’ll be required to pay back, sometimes years later.
Understanding the Work Rules
A lot of SSDI recipients want to try working again at some point, at least in some capacity. The SSA has programs specifically designed to let you do that without immediately losing everything. Understanding them before you need them is a lot better than figuring them out after the fact.
The Trial Work Period gives you nine months, within any rolling sixty-month window, to work and earn any amount while still receiving your full SSDI benefit. The nine months don’t have to run consecutively. You can work for a few months, stop, and pick back up later, and those months accumulate toward your nine without you losing benefits in between trial months.
After the Trial Work Period ends, you enter the Extended Period of Eligibility, which runs for thirty-six months. During this window you receive benefits for any month your earnings fall below the Substantial Gainful Activity threshold, the monthly income limit the SSA uses to define substantial work. Go over the limit one month and benefits pause. Drop back under the next month and they resume. No new application.
Expedited Reinstatement is the safety net for after the Extended Period of Eligibility. If benefits end because of work and your condition later prevents you from sustaining it, you can request reinstatement within five years without starting the full application process over again.
The current SGA threshold adjusts annually. Look it up at ssa.gov at the start of each year so you know exactly where the line is.
Your First Continuing Disability Review
At some point after approval, the SSA will conduct a review to confirm you still meet the definition of disability. This is called a Continuing Disability Review, or CDR. It’s standard and it happens to everyone.
When it happens depends on your condition. If improvement was expected, the review may come within the first year or two. If improvement is possible but not expected, typically every three years. If improvement is unlikely given your condition, every five to seven years.
The best thing you can do to prepare for a CDR, starting right now, is to keep consistent medical records. See your doctors regularly. Make sure your ongoing limitations are being documented at appointments, not just your symptoms. A well-maintained medical record going into a CDR makes the process significantly less stressful.
If you receive a CDR packet in the mail, respond to it completely and on time. And know that even if a CDR results in a proposed cessation of benefits, you have the right to appeal and to request that benefits continue during the appeal. That ten-day window to request benefit continuation is something to act on immediately if it ever comes up.
A Few Other Things Worth Knowing
Create or log into your my Social Security account at ssa.gov if you haven’t already. This is where you can view your payment history, update your direct deposit information, get a benefit verification letter if you need proof of income for housing or other purposes, and check on any SSA correspondence related to your account.
Benefit verification letters come up more often than you’d expect. Landlords, lenders, government assistance programs, utilities…a lot of them ask for proof of income. The my Social Security portal lets you generate one on demand without calling the SSA.
Look into other programs you may now qualify for. SSDI approval often opens doors to additional assistance. SNAP food benefits, Low Income Home Energy Assistance, state pharmaceutical assistance programs, property tax relief programs in some states. Approval for SSDI doesn’t automatically enroll you in any of these, but it often makes you eligible. It’s worth spending an hour looking into what’s available in your state.
And finally, keep copies of everything. Your approval letter, your benefit amount documentation, any SSA correspondence going forward. Store them somewhere you can find them. You’ll reference that paperwork more than you expect over the coming months and years.
The Bottom Line
Getting approved was the hard part. The first 90 days are about understanding the system you’re now in well enough to navigate it confidently. First payment timing, back pay, the Medicare gap, reporting requirements, work rules, CDRs. None of it is complicated once you know what you’re looking at.
You did the hard work to get here. Now it’s just a matter of knowing the rules of the road going forward.